Chest osteochondrosis is rare in clinical practice. It was previously diagnosed mainly in the elderly, but is now often seen in patients under 35 years of age. Pathology is more common in women than in men. This degenerative-dystrophic disease is difficult to diagnose because severe symptoms occur only in the later stages.
In addition, the symptoms of this disorder can be easily confused with signs of impaired lung and heart function. This disease cannot go untreated as it can cause curvature of the spine, the development of persistent pain syndrome and other complications that can negatively affect the quality of human life.
What is chest osteochondrosis?
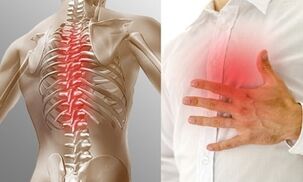
In the International Classification of Diseases, this pathological condition has the code ICD-10 - M42. Chest osteochondrosis is much less common than cervical or sacral. This is no accident. Due to the presence of a rigid rib cage in this part of the body, this part of the spine is physiologically less mobile.
The chest region contains more vertebrae than the neck and lumbar region, but the discs in this part of the spine are thinner. These anatomical features contribute to a decrease in the mobility of this part of the spine, making them less prone to injury.
However, if you are exposed to a number of harmful factors, osteochondrosis can develop. At first, there are signs of damage to a disc, but in the future, other elements may become involved in the pathological process. As the disease progresses, the bone elements and the ligaments and muscles that support the spine are damaged.
Degenerative-dystrophic processes in the thoracic region grow more slowly. For years, it is not uncommon for the fibrous rings of damaged discs to be destroyed so much that protrusions and hernias appear.
Severe clinical manifestations occur after a critical decrease in disc height and root capture. This can lead not only to abortions, i. e. , short-term pain attacks in the chest region, but also to violation of innervation of internal organs. It is much more difficult to treat pinched nerve roots in this area.
Reasons for improvement
In most cases, spinal problems do not occur suddenly. Such a disease, such as osteochondrosis, is no exception in this regard. This pathology of the intervertebral discs is the result of long-term degenerative-dystrophic processes. In most cases, it is impossible to determine exactly what caused the disorder to develop. Factors that cause the appearance of osteochondrosis of the thoracic spine include:
- congenital or acquired deformity of the spine;
- overweight;
- spinal overload during pregnancy;
- infectious diseases;
- hypothermia; metabolic disorders;
- hormonal disorders;
- chronic stress;
- bad habits;
- connective tissue diseases;
- dysplastic changes;
- postural disorders;
- unhealthy diet;
- injuries.
Destruction negatively affects the condition of the spine. People who lead a sedentary lifestyle are more likely to suffer from chest osteochondrosis. In addition, age-related changes and slowdowns in metabolism, which are observed in patients older than 55 years, contribute to the development of these disorders.
Genetic predisposition can be a factor that can trigger the development of pathology. The genes that create the conditions for the onset of thoracic osteochondrosis have not yet been identified, but they have been diagnosed more frequently in people with a family history of such disease.
Symptoms and Signs
The clinic of this condition depends on the stage of neglect of the process, the level of intervertebral disc lesions, and the age of the patient. There are no specific signs in the early stages of development, but general symptoms may occur periodically. Often, in the early stages of development, the disease occurs only with the onset of cold weather or physical overload. The initial manifestations of the development of osteochondrosis of the thoracic region are as follows:
- rapid fatigue;
- back pain and pressure;
- muscle cramps;
- cold limbs.
The patient's condition worsens as the disease progresses. Aching chest pains appear. They are especially common in the background of a prolonged stay or with sudden movements. In addition, severe pain syndrome may occur when lifting weights. Rotating the torso can cause increased pain. The presence of osteochondrosis is also indicated by the occurrence of dull pain in the shoulder blades.
Osteochondrosis of the thoracic region is often accompanied by the appearance of an abnormal bend. In severe cases, the patient may develop a lump. In addition, this disease can trigger the appearance of pain during deep breathing and exhalation.
When the nerve roots are pinched, a feeling of numbness often occurs in the upper limbs and skin of the upper body. Due to the violation of innervation and blood circulation, the feeling of a goose bump appears on the skin. Legs and hands are always cold. Limb sensitivity may be present. In advanced cases, this disease can lead to symptoms of damage to other organs as a result of violation of their innervation. In the final stage of the process, you may:
- intercostal neuralgia;
- stool disorders;
- bloating;
- heartburn and nausea;
- itching and burning in the legs;
- violation of the reproductive system;
- Asthma attacks.
As the pathology progresses, the person's ability to work decreases. Physical activity is kept to a minimum. In the future, this disorder may create preconditions for the development of serious complications. Increases the risk of abnormal fractures. The curvature of the spine leads to compression of the organs in the chest.
Adverse disease is associated with damage to the heart muscle and loss of lung volume. Most often, such severe complications are accompanied by widespread osteochondrosis involving multiple intervertebral discs at the same time.
Degree of chest osteochondrosis
The existing classification divides the development of this pathological condition into 4 degrees. Each is made up of intervertebral discs, vertebrae, and other elements that make up this part of the spine.
First degree
There are no pronounced clinical manifestations in the first stage of pathology, but specific changes in the structure of intervertebral discs can already be revealed by a comprehensive diagnosis. The fibrous ring, which receives less moisture and nutrients, gradually loses its elasticity. Tissues often form microcracks into which the nucleus pulposus is squeezed. Displacement of the discs into the spinal canal is possible. Protrusions are formed. There are no signs of cracking of the annulus fibrosus.
Second Grade
With the second-degree transition of the disease, the first clinical manifestations are observed. Patients occasionally experience pain and other neurological symptoms. During specific diagnostics, there are signs of decreased elasticity of the tissues that make up cyclic fibrosis. The cartilage will be very thin, leading to an increased risk of hernia. The height of the intervertebral plates decreases, causing the structure of the spinal column to acquire abnormal mobility.
Third Degree
In the third stage, the changes in the structure of the discs become so pronounced that the first signs of kyphosis or scoliosis appear. Often at this stage of the process, the damaged annulus fibrosus is interrupted. This phenomenon is accompanied by the exit of the pulse of the nucleus beyond the disc. The resulting hernia, depending on the direction of protrusion, can compress the nerve roots or spinal cord. Severe pain and neurological disorders occur. Spinal mobility increases, creating conditions for injuries and fractures.
Fourth grade
With the fourth-degree transition of pathology, the structure of the intervertebral discs is so disturbed that the damping function ceases. The annular fibrosus and the nucleus pulposus lose their elasticity. These elements begin to ossify. Violation of the damping function of the plates affects the vertebrae, which carry too much load.
At the edges of the vertebrae adjacent to the damaged disc, osteophytes, or bone growths, begin to grow rapidly. The surrounding ligaments are involved in the pathological process. They lose their elasticity and no longer support the spine properly. In addition, at this stage in the development of the pathological process, the work of the muscle device is interrupted.
Set up a diagnosis
If signs of this disorder develop, the patient should consult a neurologist and orthopedic surgeon. First, the doctor performs an external examination and collects a medical history. Laboratory tests often prescribed to diagnose the disease include blood and urine tests. An X-ray is taken to obtain information about spinal structure defects. This research reveals:
- reduce the height of the disc; edges of
- elements;
- hernia;
- changes in vertebral bodies; They form
- osteophytes and so on.
Discography is assigned to clarify disk structure errors. This study makes it possible to identify the uneven contours of the pulposus nucleus, to assess the extent of disc destruction and the decrease in tissue density. CT and MRI are often done for better imaging. Given that the clinical manifestations of thoracic osteochondrosis are similar to those of coronary heart disease, electrocardiography is often prescribed to distinguish these conditions.
Management Options
This condition requires complex treatment. First, patients are selected for medications that help eliminate symptomatic manifestations and improve the nutrition of intervertebral discs. Medication should be supplemented with physiotherapy and exercise. You can use some folk remedies as a supplement. In addition, it is recommended to follow a specific diet.
Medications
In patients with severe pain syndrome, it is recommended that the patient maintain bed rest. This reduces the intensity of the pain. Painkillers and NSAIDs are often prescribed to eliminate discomfort. If the pain syndrome occurs too intensively, blockage may be required. Glucocorticosteroids are often prescribed to relieve pain in this disease.
Chondroprotectors are prescribed to improve the nutrient and water saturation of intervertebral discs. In some cases, antispasmodics and muscle relaxants are prescribed in short courses. These medications help relieve muscle cramps. If necessary, diuretics are prescribed to eliminate soft tissue edema. To improve the condition of nerve endings exposed to compression, the patient needs B vitamins.
Physiotherapy and massage
Therapeutic practice and massage are the most important elements in the treatment of osteochondrosis, but can only be used after medication suppression of symptoms. Properly chosen exercises will help improve lung ventilation and strengthen the muscular corset that holds the spine.
First, all the necessary exercises should be learned under the supervision of a movement therapy instructor. In the future, the patient can perform exercises at home. People with such a disease are advised to attend the pool.
Massage helps eliminate muscle hypertension and improve soft tissue nutrition. In order for the procedures not to cause damage, they must be performed by a professional. In most cases, a classical massage is performed, which involves successive rubbing, smoothing, and tightening of the problem area. Acupressure and segmental massage can have great benefits. These techniques include the effect on pain points. They help improve blood circulation and lymphatic drainage. In most cases, it is sufficient for patients to undergo procedures 2-3 times a week.
Acupuncture
This method involves placing needles in areas of the patient's body. This method allows you to quickly eliminate muscle cramps and pain. Acupuncture procedures should be performed by a specialist in this matter. If a professional does this, the procedure will be almost painless. Acupuncture is contraindicated in people with oncological diseases and mental disorders. It is not recommended to use this method for the treatment of osteochondrosis in the presence of severe inflammatory processes.
Manual therapy
Manual therapy helps to restore the correct anatomical position of the vertebrae. In addition, this method helps reduce the intensity of pain and muscle cramps. This effect helps to restore the ligament device. Such procedures can slow the development of this pathological condition. The duration of manual therapy is chosen individually by the patient.
Post-isometric relaxation technique
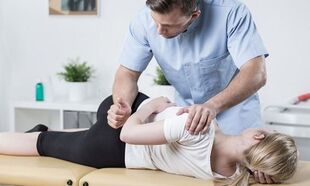
Post-isometric relaxation is a special technique that involves tightening and then relaxing all the muscles surrounding the spine.
Such exercises should be performed under the supervision of a professional who can assess the correctness of the movements and the severity of the muscle tension. This method allows you to quickly eliminate pain and restore the normal functioning of the muscle and tendon ligaments.
Folk remedies
It is impossible to treat osteochondrosis with folk remedies alone, as this approach can exacerbate the course of the disease. It is best to use a variety of preparations based on herbs and other natural ingredients to supplement traditional therapies. Before you start using it, you should get a doctor's recommendation about the appropriateness of using that or another folk medicine.
Celery root
Properly cooked celery root is believed to help saturate cartilage with nutrients and water. To make the product, 1 root must be thoroughly chopped and poured with 1 liter of boiling water. You should stick to the composition for at least 8 hours. After this time you need to filter the product and 1 tsp. 3 times daily before meals.
Sunflower root
Sunflower root decoction is often used to treat osteochondrosis of the cervical spine. To make the product you will need about 1 cup of chopped herbal ingredients, pour 3 liters of water. The mixture should be boiled for 3-5 minutes. The substance should then be cooled and taken in the form of tea for several days. Honey can be added to improve the taste of the drink. It is better to store the rest of the medicine in a thermos.
Home ointment
A simple homemade ointment can be used for osteochondrosis rubbing. To prepare the product, about 150 g of lard must be melted in a water bath. Then add 2 tablespoons. l. natural wax.
Boil the product for at least 20 minutes. Then add 1 tablespoon to the heated mixture. l. pine oil. The product must be boiled for another 20 minutes. Last but not least, 2-3 minutes before removing the container from the heat, add 1 tablespoon to the mixture. l. ammonia. The finished composition should be divided into jars. Store the homemade ointment in the refrigerator.
Nutrition for chest osteochondrosis
Patients with osteochondrosis of the thoracic region need a balanced diet. Adequate amounts of protein-rich foods should be included in the diet. It is advisable to consume foods high in chondroitin on a regular basis, including fish aspic, gelatinous meat, and so on. It is essential to include fermented dairy products, vegetables and fruits in the diet. Food should be steamed or baked. Fatty and fried foods should be avoided. It is advisable to take food in small portions, but often. This will prevent overeating.
Aggravation: what to do?
It is desirable to minimize activity during the acute period of the disease. If possible, avoid poses in which pain syndrome is exacerbated. First aid for the worsening of osteochondrosis involves the use of medications that reduce the severity of edema, inflammation, and pain. The patient is advised to rest in bed. It is advisable to follow a gentle diet during this period. You can only start exercising and physiotherapy after the symptoms have stopped.
Forecast
This disease can now only be cured at an early stage of development. In case of late diagnosis, therapy is aimed at eliminating the symptoms and improving the mobility of the spine. In some cases, surgical treatment is required. With an integrated approach to therapy, a person with this pathology can lead a full-fledged lifestyle without experiencing pain and other neurological disorders.
Prevention
To prevent this condition, it is advisable to avoid sudden heavy lifting. You should always dress appropriately for the weather, avoiding hypothermia. In addition, to prevent osteochondrosis, you must fight hypodynamics and monitor posture. As part of the prevention of this pathology, it is recommended to eat correctly and monitor your weight carefully.

























